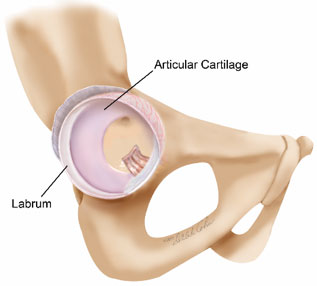
The labrum is important for protecting the articular cartilage. The labrum has excellent healing capacity and tears can be repaired with successful results. The articular cartilage has less recuperative ability, and thus with most joint preserving surgical procedures, the severity of the articular damage is a limiting factor on the success of the operation.
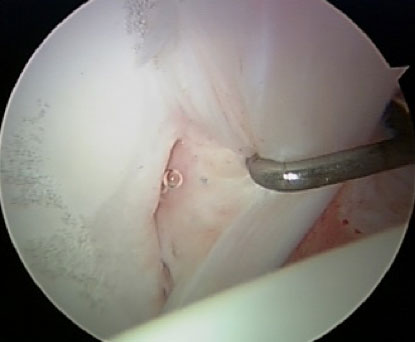
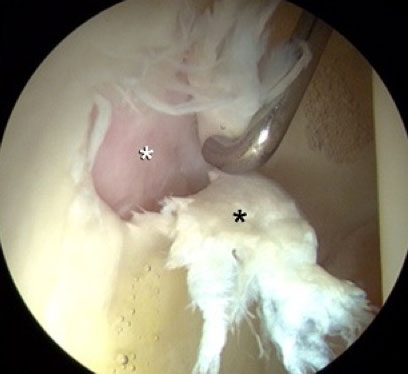
Imaging studies, such as MRI, are pretty reliable at showing damage to the labrum, but often unpredictable in their ability to discern whether there is damage to the articular cartilage. With arthroscopic surgery, it is often only at the time of surgery that the severity of this articular damage can be determined. Our experience over more than a quarter of a century shows that most labral tears will have some accompanying articular damage. Thus going into surgery, the articular cartilage may be the wild card on the success of the procedure. This will only be fully known at the time of surgery.
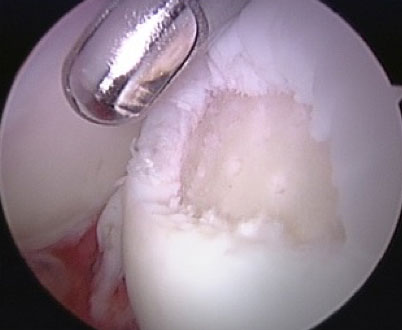
The labrum can simply be sutured back to the rim of the acetabulum and will heal. The articular cartilage is usually just polished (“chondroplasty”) to try to smooth roughness as best as possible. Some areas of articular cartilage that have flaked off down to exposed bone can be treated with a technique called microfracture. This is simply a process of creating small perforating holes into the bone that establish vascular connections to the cartilage defect, stimulating fibrocartilaginous healing. Fibrocartilage is not perfectly normal cartilage, but it is the body’s best attempt at healing. It is imperfect, but much better than leaving the raw bony surface to rub against the opposite side of the joint. Creating these small perforation in the bone adds very little to the surgery, but does require an altered rehabilitation strategy following the operation. The initial healing tissue is like an immature scab. If the scab is not protected, it will repeatedly break open, and the healing is less complete. Thus, protected weightbearing with crutches may be necessary for eight weeks following the surgery. Although imperfect, in our experience, the results of microfracture to create fibrocartilage can be quite successful. The geometry of the hip joint is such that this operation works much better than in other joints like the knee.
A normal, healthy hip joint is a very durable structure that can withstand hard use. Most commonly when injury or damage occurs, there is some underlying abnormality of the way the joint is formed making it more susceptible to damage. By far, the most common cause is femoroacetabular impingement (FAI). Second on the list is dysplasia. However, some patients can present with a hybrid condition of both dysplasia and impingement that must both be carefully weighted to determine which or what combination of treatment strategies must be employed.
There are also inflammatory types of arthritis that do not necessarily involve bony structural abnormalities of the joint. The synovium is a membrane that lines the hip, normally producing synovial fluid that lubricates the joint, providing nutrition. With inflammatory types of arthritis, the synovium grows out of control, eroding the articular cartilage leading to arthritis. Occasionally, arthroscopy for resecting the synovium (synovectomy) can be beneficial. This is not frequently necessary because in recent years pharmacological management to control the synovium have made significant advancements.
Location
2004 Hayes Street
Suite 700
Nashville, TN 37203
Office Hours
Monday-Friday:
8:00 am – 5:00 pm